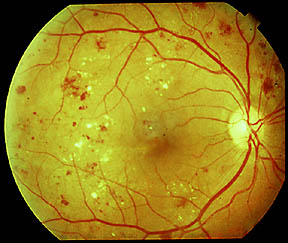
This case represents atypical retinopathy, likely resulting from the combination of idiopathic aplastic anemia in a patient with concomitant diabetes but no previous evidence of diabetic retinopathy. Unfortunately, the patient died three weeks later from acute intracranial hemorrhage. He returned to my office the following week to tell me he had been diagnosed with aplastic anemia and was started on several new medications, including cyclosporine A and prednisone. 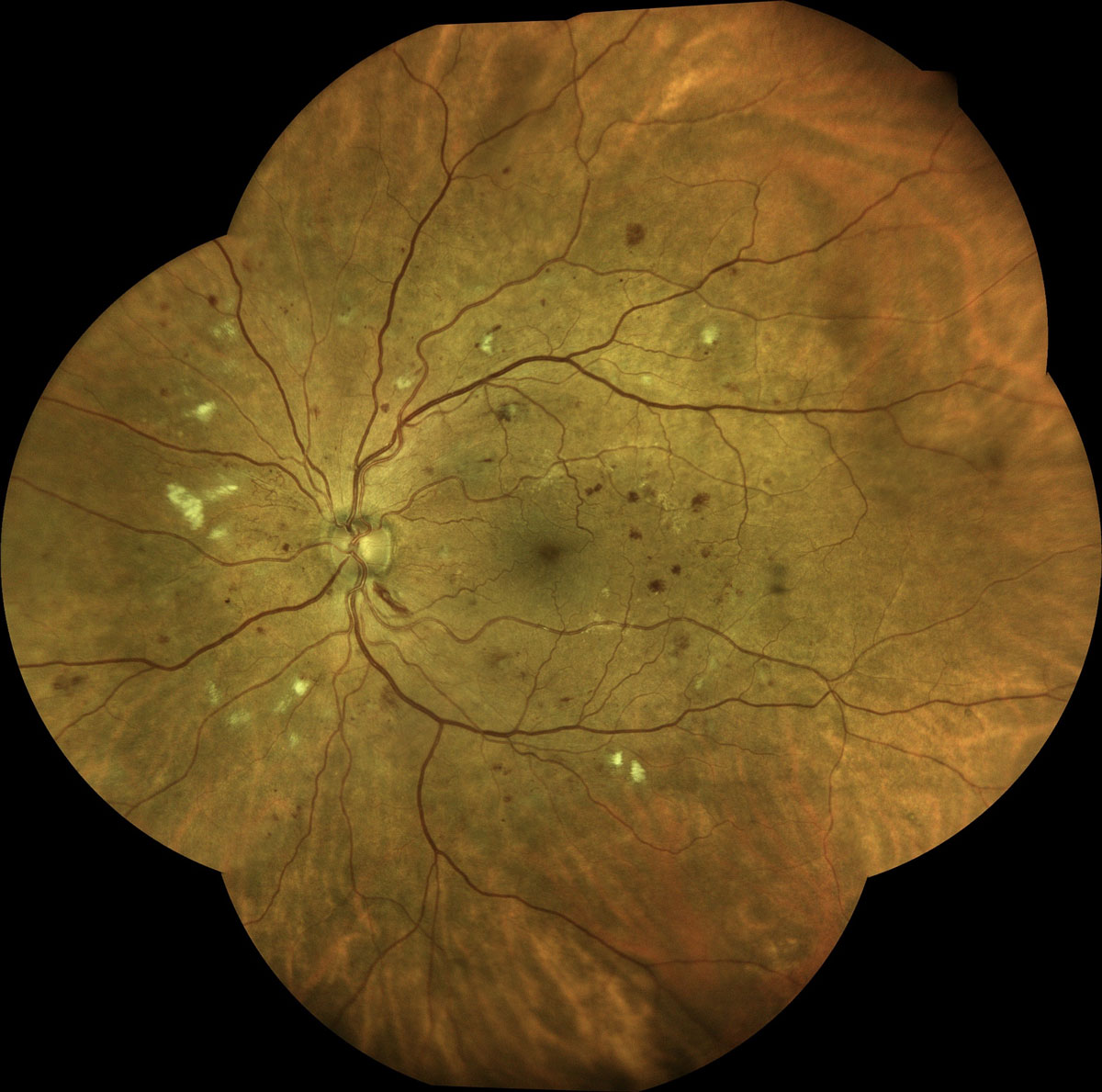
His vision and retinas remained unchanged. I sent a report to the patient’s internist and asked him to return in eight weeks.Īt the next follow-up, the patient reported he had been hospitalized twice in those eight weeks for severe anemia, receiving multiple transfusions and referral to hematology. Moreover, the HbA1c error message and self reported malaise/dypsnea made me suspect a hematologic disorder. The white-centered hemorrhages, though, were less typical of diabetic retinopathy and careful review of previous fundus imaging showed no retinopathy whatsoever. Given the fundus appearance and clinical history, moderate, non-proliferative, diabetic retinopathy as well as predominantly peripheral, diabetic retinopathy lesions (PPL), both risk factors for sight-threatening diabetic retinopathy, seemed probable. I performed in-office glycosylated hemoglobin (HbA1c, A1cNOW, PTS Diagnostics) which gave the following error reading “the blood sample may have too little hemoglobin (Hb) for the test to work properly.” A spot glucose reading was performed and measured 161 mg/dl. Spectral domain optical coherence tomography was performed to rule out subclinical macular edema, and was ‘normal’ and unchanged compared to SD-OCT captured a year earlier. 
Closer inspection of the images showed a few intra-retinal hemorrhages with a white center. Montage ultrawide-field retinal imaging confirmed predominantly peripheral retinopathy, right eye more than left (see Figure 1). Related: Look at the retina in a different way I did not detect retinal thickening with a fundus lens. A dilated fundus exam showed dot and blot hemorrhages in the posterior pole, which appeared far more numerous in the mid-peripheral retina with BIO exam. Intraocular pressure measured 19/18 by applanation. Both lenses showed early nuclear sclerosis and the irides were normal. Corrected acuities were again better than 20/20, with minimal refractive change. His current medications included losartan, feonfibrate, and metformin and he noted a an internal medicine doctor’s diagnosis of diabetic peripheral neuropathy but no evidence of kidney dysfunction. His previous eye exam from one year earlier, showed no diabetic retinopathy and mild nuclear sclerosis in each eye with best-corrected visual acuities of 20/20+. He reported that his diabetes arose 10 years ago and that his HbA1c was “good” but he felt unusually tired the last several months and was having trouble catching his breath. Reduced Hb levels in this patient made accurate HbA1c analysis impossible, but an error message that arose in testing pointed to an underlying etiology of the patient’s symptoms.Ī 72-year-old male with type two diabetes came to my office for a dilated retinal examination. A diabetic patient presented with atypical retinopathy, likely resulting from the combination of idiopathic aplastic anemia and concomitant diabetes.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
